Why Your Belly Fat Persists Even When You’re Doing the Right Things
Sleep, stress, menopause, medications and other overlooked reasons a stubborn waistline may have little to do with willpower
You’ve been watching what you eat. Cutting back on the snacks. Making the kind of earnest, grown-up dietary decisions that really ought to count for something. And yet, the waistline isn’t budging.
If that sounds familiar, you’re not alone. I’ve had a number of messages from readers lately saying exactly this: they’ve been paying attention to their diet, doing the right things, and their waist measurements haven’t shifted. That’s frustrating. And I get it, because the assumption most of us start with is simple: belly fat is a food problem, so the fix must be a food fix.
But what if that assumption is only partly right?
If you’ve been following this series, you’ll know my own waistline expanded after a few too many fast-food lunches with a friend who was bulking up. Fixing my diet brought it back. So yes, food matters.
But today’s point is that an expanding waistline isn’t just a food story. It’s also a sleep story, a stress story, an activity story, sometimes a hormone story, and occasionally a medical one.
Your waistline is listening to more than your fork. Annoyingly, it also seems to care about your sleep, your stress levels, and whether you’ve spent the day glued to a chair.
Why does this matter?
Because visceral fat isn’t just the padding that changes how your waistband fits. It’s the fat packed around your abdominal organs, and higher levels are linked with a greater risk of insulin resistance, type 2 diabetes, fatty liver disease, heart disease, and earlier death.
In other words, this isn’t mainly a cosmetic issue. A growing waistline can be an early sign that something more important is shifting under the bonnet.
If you missed the earlier pieces in this series, you can find them, along with all previous issues of One Health Tweak a Week, on the homepage.
So what are the other drivers? And how much do they actually matter?
Sleep: duration, quality, and regularity
Let’s start with the factor that has the strongest evidence: sleep.
In a study of 5,151 Americans aged 18-59, researchers found a clear link between insufficient sleep and increased visceral fat. The shorter the sleep, the more visceral fat. For women, the benefits plateaued at around 7.5-8 hours; for men, longer sleep was associated with progressively less visceral fat.
But it’s not just short sleep that’s the problem. A larger cross-sectional survey of over 112,000 Americans found that both insufficient and excess sleep were associated with more visceral fat. The sweet spot? Around 7.5-8 hours. Sleep less than that or more, and visceral fat levels were progressively higher. You can see this in the U-shape of the graph below.
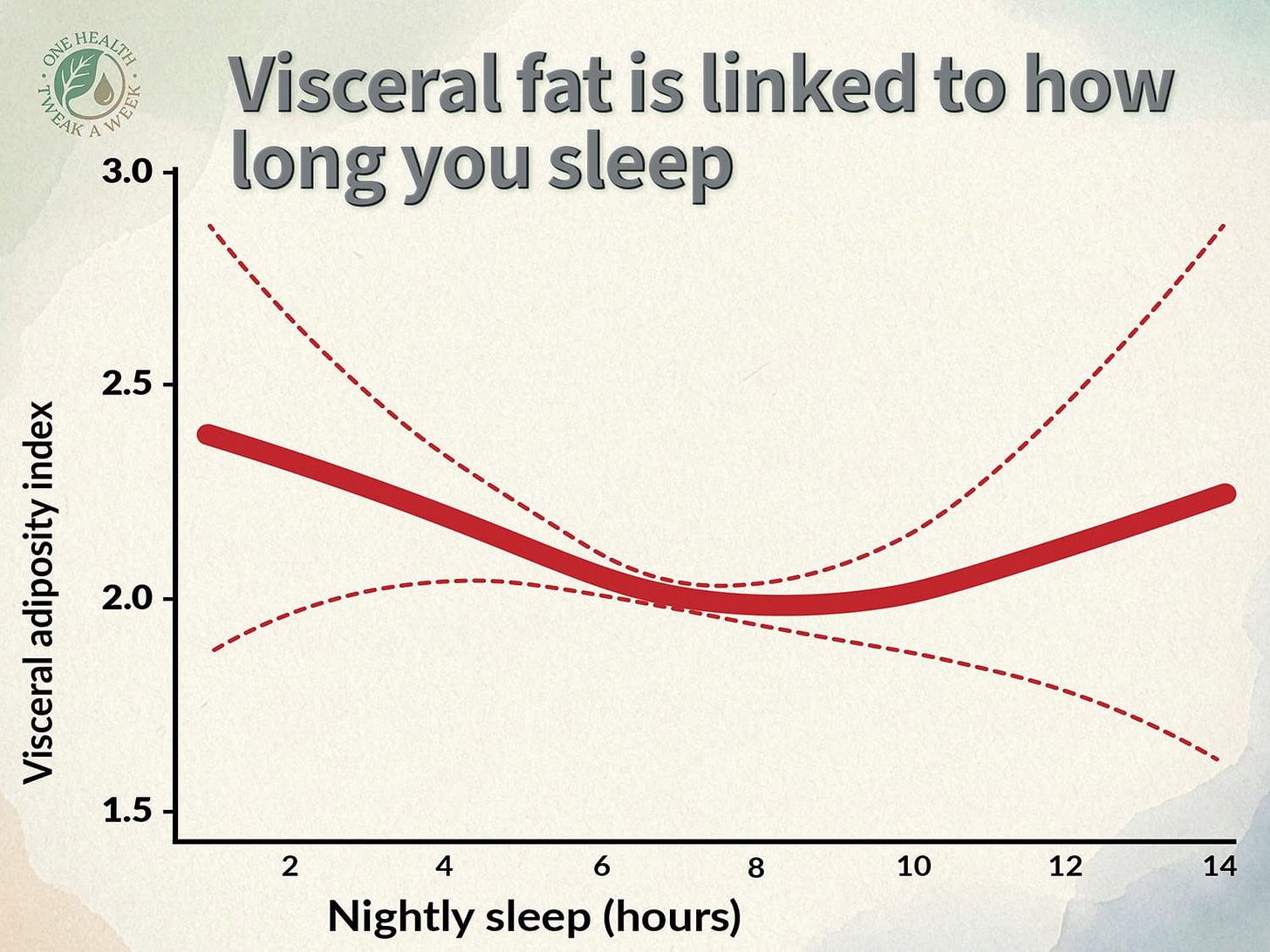
A five-year study of Hispanic and African Americans told a similar story: sleeping for less than five hours, or for eight hours or more, was linked to greater accumulation of visceral fat, though the association was limited to those under forty.
What’s striking is how quickly this can happen. In a small but tightly controlled experiment, 12 healthy young adults had their sleep restricted to four hours per night for just two weeks. The result? A measurable increase in visceral fat. Two weeks. That’s not a slow drift: that’s your body making administrative decisions you did not approve.
And it’s not just how long you sleep. It’s how well and how consistently.
Chinese researchers followed almost 400 young adults for a year, with each participant wearing a sleep monitor for a week at baseline. The more their sleep was fragmented, the more visceral fat they accumulated over the following twelve months. And in a study of 277 teenagers, irregular sleep and wake times and social jetlag (those weekday-to-weekend schedule shifts most of us know well) were linked to increases in visceral fat.
So, the message from the sleep research is consistent: aim for about 7-8 hours of good-quality sleep, and try to keep your schedule steady through the week. Lie-ins at the weekend might feel restorative, but if your sleep schedule is pure improvisation, your metabolism will notice.
Stress, depression, and loneliness
Now let’s move from the bedroom to the mind. Because what’s going on in your head seems to matter for what’s going on around your waist.
In a study of Finnish twins where one was lean, and the other had obesity, researchers found markers of chronic stress in the twins with greater visceral fat, including elevated cortisol levels. Because these were identical twins, genetics was effectively held constant, which makes the stress signal stand out as an important factor.
A seven-year study of over 2,400 midlife Dutch adults found that experiencing three or more stressful life events was linked to increases in waist circumference. Not dramatic changes, but steady, cumulative ones: exactly the kind that creep up on you.
The relationship may run both ways. A review of the evidence suggests that while stress increases the likelihood of obesity and visceral fat gain, visceral fat itself can raise cortisol levels, potentially making people more susceptible to future stress.
In other words, stress feeds belly fat, and belly fat feeds stress. Not a great loop to be caught in.
Depression follows a similar two-way pattern. The metabolic effects of increased visceral fat appear to directly affect the brain, increasing the risk of depression. At the same time, depression is associated with behaviours that drive visceral fat accumulation: emotional eating, inactivity, and disrupted sleep. Each side of the equation can sustain the other.
And then there’s loneliness. A large Norwegian study found that loneliness in adolescence tripled the risk of abdominal obesity in adulthood in women, and increased it more than fivefold in men. Fivefold. Plausible mechanisms include emotional and irregular eating, excess snacking, reduced physical activity, and the effects of chronic stress hormones.
None of this means feeling stressed or lonely causes visceral fat in any simple way. These are associations, and the pathways are tangled. But the consistency of the pattern across studies and populations makes it hard to ignore: your emotional life isn’t separate from your metabolic one.
Inactivity and sedentary behaviour
This one probably won’t surprise you, but it’s worth seeing the numbers.
During the COVID lockdown in Japan, researchers tracked activity levels using accelerometers. As you’d expect, sedentary time went up. And so did visceral fat, as the graph below shows.
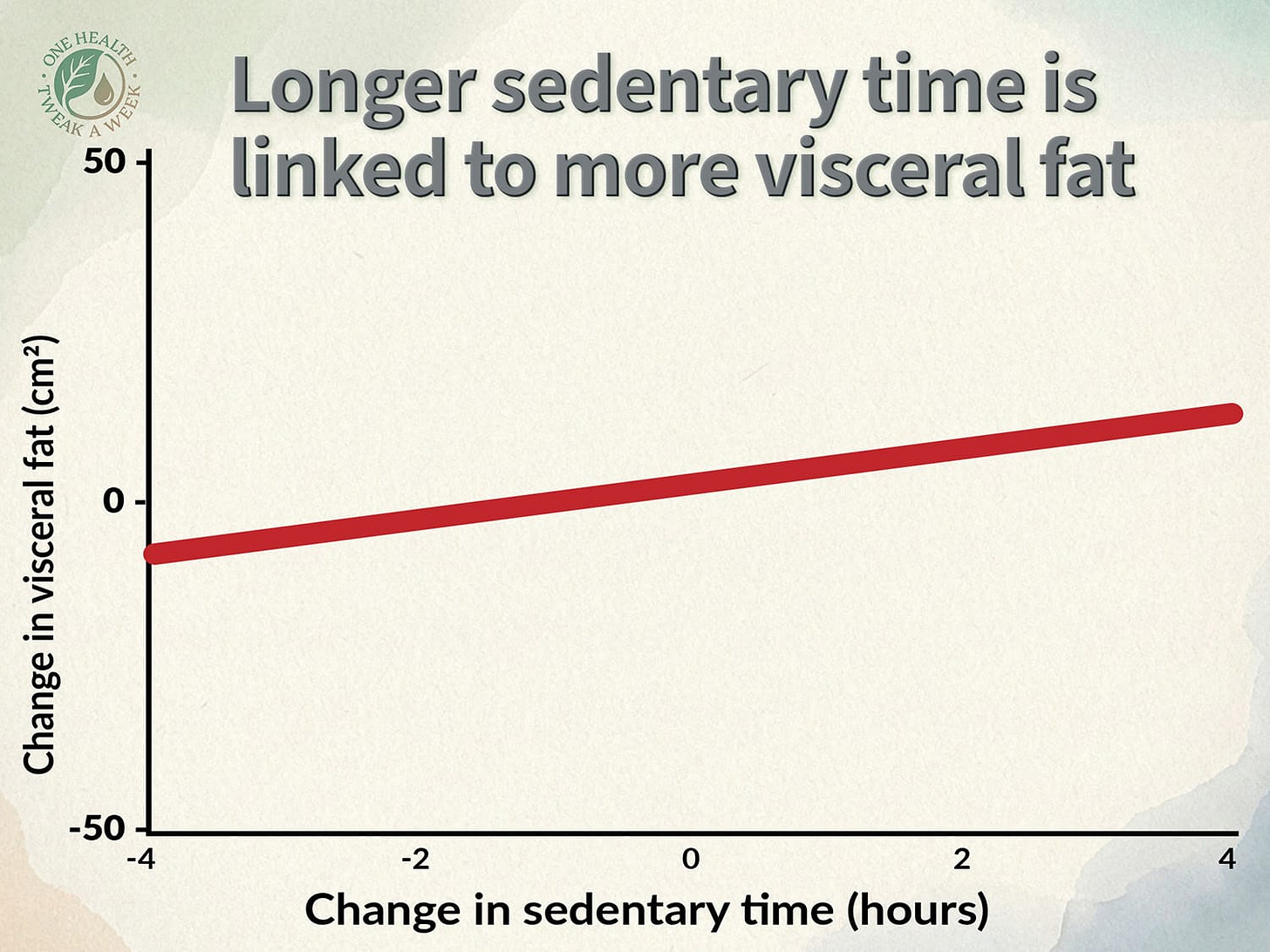
The effect was relatively modest, but there’s something quite encouraging here: you don’t need vigorous exercise to shift the needle. Just being less sedentary, spending less time sitting, was associated with less visceral fat gain. That’s a lower bar than constructing an entirely new personality around the gym.
That said, moderate to intense exercise does seem to have a particular advantage here. Visceral fat is more metabolically responsive to exercise than subcutaneous fat: adrenaline released during harder exercise preferentially shifts fat from visceral stores. So serious exercise matters. But simply moving more also counts.
Brazilian researchers found that people getting fewer than 150 minutes of physical activity per week were 2.3 times more likely to have excess visceral fat. Only a quarter of participants in that study hit the 150-minute mark. If you’re not there yet, that’s a clear, achievable target.
So, yes, harder exercise seems especially good at shifting visceral fat. But this is not an all-or-nothing story where anything short of intervals and kettlebells is worthless. Your waistline appears to notice both the exercise you do and the sitting you stop doing. If vigorous workouts are not realistic right now, simply becoming a person who moves more and sits less is still likely to be a meaningful step in the right direction.
If you know someone who’s trying to improve their long-term health, please let them know about One Health Tweak a Week.
The other contributors: menopause, sleep apnoea, and medication
Some drivers of visceral fat are physiological or medical rather than purely behavioural, and they’re worth knowing about because they can explain why your best dietary efforts aren’t working.
Menopause is one of the most significant. It’s very common to gain weight around this transition. Energy expenditure falls. About two years before the final period, the rate of fat gain doubles. And even for women who don’t gain weight, falling oestrogen levels lead to a redistribution of body fat, with an increase in visceral fat. Postmenopausal women have, on average, 50% more fat around the abdominal organs than premenopausal women.
Sleep apnoea creates its own vicious circle. Obesity, especially abdominal obesity, is a key driver of sleep apnoea. But as we’ve seen, disturbed sleep is itself linked to increased visceral fat. Each problem feeds the other.
And some medications are associated with increased abdominal fat. Steroids are a common culprit, along with some antipsychotic medicines, SSRI and tricyclic antidepressants, and certain epilepsy and HIV drugs. If you suspect your medication might be contributing, talk to your doctor rather than adjusting anything on your own.
A word on the evidence
Much of what we’ve covered today is observational. That means the findings depend on the accuracy of participant-reported information, and other factors may affect results. Researchers work hard to account for confounders, but it’s always possible that some influence remains.
That said, the sleep evidence has the strongest causal signal: experimental sleep restriction has directly increased visceral fat in controlled settings. For stress, depression, and loneliness, the evidence is more associative but remarkably consistent across populations, ages, and geographical regions. And the overall picture is corroborated by studies that use objective measures rather than self-reports.
What this means for your health
If you’ve been focused on food and your waistline still isn’t shifting, it doesn’t mean you’re failing. It may mean you’re only pulling one of several levers.
A better question is not just, What food am I eating that I shouldn’t be? It’s: What has changed in the bigger system? Are you sleeping less, or later, or more erratically? Are you under chronic stress? Feeling low? Moving less? Going through menopause? Snoring like a chainsaw and waking unrefreshed? On a medicine that has quietly changed the rules?
The evidence points clearly to a broader set of inputs: sleep, stress, mood, activity, hormonal changes, sleep disorders, and medication. Some of these are fully within your control. Others need a conversation with your doctor. But recognising that visceral fat isn’t just a food story is the essential first step, because it changes what you do next.
Instead of tightening your diet yet again, think of it less as a discipline problem and more as a detective job. Which of these other factors might be working against you?
As always, your responses are anonymous, but they really help me tailor future content to what’s most helpful to you. Please take a moment to click a button.
HEALTH TWEAK OF THE WEEK
Visceral fat isn’t just the padding that changes how your clothes fit. It’s the fat packed around your abdominal organs, and higher levels are linked to insulin resistance, type 2 diabetes, fatty liver disease, heart disease, and earlier death.
The important point is that it isn’t driven by food alone: sleep duration and quality, stress, mood, physical activity, hormonal changes, sleep apnoea, and some medications can all nudge it upwards.
If your waistline isn’t responding to diet alone, the answer may not be stricter eating. It may be time to stop blaming your lunch for things your sleep schedule, stress levels, or wider physiology had a hand in.
1. Prioritise 7.5-8 hours of consistent, good-quality sleep. That means keeping sleep and wake times steady through the week, including at weekends. Social jetlag and fragmented sleep are both linked to increased visceral fat. If your schedule is erratic, start by anchoring your wake time and working backwards.
2. Move more, and aim for at least 150 minutes of moderate activity per week. People falling below that threshold were 2.3 times more likely to have excess visceral fat. But even reducing sitting time, without structured exercise, is associated with less visceral fat gain. Walk more. Sit less. Build from there.
3. Take stock of stress, mood, and connection. Chronic stress, depression, and loneliness are all linked to increased visceral fat through both biological and behavioural pathways. This isn’t a “think positive” platitude. It’s a practical prompt: if stress is chronic, explore what helps (exercise, time outdoors, meditation). If low mood or loneliness is persistent, talk to your doctor.
And if you’re going through menopause or suspect sleep apnoea or a medication effect, that’s a conversation worth having with your doctor, too.
A stubborn waistline doesn’t always need a stricter diet. Sometimes it needs a wider lens.
🎧 Want a smart listen for your next walk, drive, or mildly reluctant bit of exercise?
🎙️ This week’s One Health Tweak a Week podcast is about the non-food factors that quietly push fat towards your middle - the fat around your organs that matters far more to your long-term health than how your jeans happen to fit this week.
In this episode, we dig into:
Why a growing waistline is not just a food story
Why too little sleep, too much sleep, broken sleep, and erratic sleep timing can all work against you
How stress, low mood, loneliness, and inactivity can quietly nudge visceral fat upwards
Why menopause, sleep apnoea, and some medications can make your best dietary efforts look oddly ineffective
We’ll also talk through why this matters for your metabolic health, why the answer is not always stricter eating, and how to think more clearly about a stubborn waistline when your lunch may not be the main culprit.
👉 Ideal listening for your next walk, commute, or while doing something wildly radical, like going to bed on time.
(Episodes are free. Paid subscribers help fund the time and tools I’m building to help turn these weekly tweaks into habits that actually stick.)
🧭 Before you go
💬 If this all sounds familiar, tell me which non-food factor you think has been quietly working against you. Sleep? Stress? Too much sitting? An erratic routine? Think of the comments as a place to compare notes.
📤 If someone in your life is eating reasonably well but still wondering why their waistline won’t shift, send this their way.
👥 Paid corner - If you’re trying to work out which of these factors is most likely to be driving your waistline, drop me a note in our private chat, and we’ll think it through together.
Until next Saturday - your waistline may be reacting to more than your lunch. It’s worth listening a little more carefully.
– Ben





